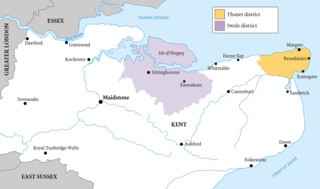
In October last year the number of people infected with Covid-19 began to rise in the coastal towns of north-east Kent. The area had escaped the full impact of the first wave of the pandemic in the spring, with many residents saying that they didn’t know anyone who had caught the virus. After the end of the lockdown on 4 July, there was a sense that the crisis was over and there was little alarm when the number of infections started to climb. The worst affected districts were Thanet, which includes the towns of Margate, Broadstairs and Ramsgate, and Swale, further west, whose main population centres are Sittingbourne, Faversham and the Isle of Sheppey, just offshore. In November case numbers rose steeply and soon north-east Kent had the highest infection rates in the country. By the middle of the month the council ward of Sheppey East, on the Isle of Sheppey, had an infection rate of 1917 per 100,000 – seven times the level in the UK as a whole.
The lockdown, with its complicated system of different tiers for different regions, appeared to suppose a virus of limited mobility with a high respect for municipal boundaries. But it was becoming clear that, whatever the effectiveness of lockdown in other parts of the UK, it wasn’t working in this corner of Kent. The surge in infections moved inexorably inland towards where I live in Canterbury, fifteen miles from Margate and ten miles from Faversham.
It wasn’t surprising that Swale and Thanet should be badly affected: these are areas notorious for their poverty and likely to provide an ideal breeding ground for the virus. They are prime examples of coastal Britain, depressed places where failed hotels and B&Bs have been chopped up into one-room flats and where few can work from home because their jobs won’t allow it; the homes, in any case, are too small to work in. Years of austerity had already cut back the funding and benefits on which such towns depended. People were vulnerable to the virus here because their health was poor before the pandemic and their access to healthcare limited: in Swale the ratio of GPs to residents is lower than anywhere else in England. Inequality is extreme: a woman living in the most affluent ward in Thanet will live on average 22 years longer than a woman living in the most deprived ward.
I found it a little comforting to reflect on factors favourable to the spread of the virus in the coastal towns of Swale and Thanet that might not apply to an inland city like Canterbury. At the east end of the Isle of Sheppey there are three prisons, with some three thousand prisoners, where an outbreak of Covid-19 was known to have taken place. Many people insisted that the prisons must be the reason the rate of infection was so high on the island – though a public health official said that only 20 per cent of infections locally had been recorded in prisons and care homes. Another explanation for the epidemic was that it had to do with immigrants. Thanet was once the heartland of Ukip, the only place where the party won control of the local council. Margate residents complained about immigrants holding parties, mingling in the streets without masks and blowing their noses unsafely. ‘You get fed up with hearing people say they [the immigrants] are bringing it in,’ Ivor Riddell, a railway conductor and trade unionist, told me. ‘It’s all part of their silver bullet belief that if we got rid of the migrants, we could get back to the 1950s.’
Some of these explanations sounded credible, others an obvious piece of scapegoating – but they turned out to be equally incorrect. By late November the epidemic was spreading fast along the Thames Estuary through Medway, Gravesham and Dartford to the west, and south towards Canterbury and Maidstone. Public health officials promised a ‘deep dive’ into the reasons for the deteriorating situation, but they appeared baffled, recommending only that people stick more rigorously to the restrictions. In London the scientists directing the national response to Covid-19 were similarly perplexed as to the reason the lockdown was working as expected in the country at large but not here.
A new variant of the virus had been detected in Kent as early as 20 September but its capabilities had not yet become visible. Eventually the levels of infection brought it to general attention. ‘This variant became of interest,’ Peter Horby, the chairman of the government’s New and Emerging Respiratory Virus Threats Advisory Group (NERVTAG), said on 23 December, ‘because there was an investigation of the increasing case numbers in Kent in early December, despite the national lockdown.’ By then it was too late to try to confine it. The new strain was already rampant and swiftly displacing the original virus in Kent, London and across the South-East. On 18 December, NERVTAG concluded that the variant had ‘started in Kent, probably from one person, and then expanded’. They also estimated that it was between 30 and 70 per cent more infectious than the original strain. By the last week of December, what was becoming known as ‘the Kent variant’ – its scientific name is B.1.1.7 – was dominant in England. By February it had spread to 83 countries and had been detected even in New Zealand, which had so far successfully suppressed Covid-19; in the US, scientists expected it to become the dominant variant by March.
NERVTAG gave no details about where in Kent the variant was first located, but the Covid-19 Genomics UK Consortium said that a key sample came from a patient living ‘near Canterbury’. A medical source, who wanted to stay anonymous, told me that the variant was first identified in Margate and came from someone with a weak immune system. Some in Kent jibbed at the prospect that the new virus would be known to history as ‘the Kent variant’, drawing a parallel with Trump’s ‘China virus’ or the ‘Spanish flu’ that didn’t even come from Spain (it first reached epidemic level in military training camps in the US).
It would be difficult to find a place where coronavirus was more likely to flourish and to enhance its mode of attack than Thanet and Swale. As in much of coastal Britain, few of the towns here are still working ports or seaside resorts. What industry there once was is largely gone, taking with it the few well-paying jobs. Of the fifteen most deprived neighbourhoods in Kent, seven are in Thanet and six in Swale. ‘We lost the mining industry and Ramsgate harbour, which was a big employer,’ the Labour councillor Barry Lewis says, lamenting the repeated blows to Margate over the past forty years. The hotel and tourism industries collapsed ‘when everybody started going abroad for their holidays’. The last big manufacturer in the area was the Pfizer plant near Sandwich, which closed in 2011 with the loss of 1500 jobs. The jobs that remain are often on zero-hours contracts. A map showing areas of maximum deprivation fitted neatly over one showing high rates of viral infection.
Everything about the average working life of someone in Swale or Sheppey puts them at risk. Much of this is to do with the need to go out to work. As Jackie Cassell, a public health specialist at the Brighton and Sussex Medical School who grew up on Sheppey, put it, ‘poverty is a mechanism for increasing social contact.’ People on the island are more likely than the population at large to use public transport to get to work, doing shifts of eight or more hours a day in warehouses or on construction sites. And people with little money are more likely to look after sick or ageing relatives. In a study of working patterns, Cassell found that on average someone who goes out to work has twelve prolonged or close periods of contact with people and seventeen brief or distant ones; those working from home have only two close or prolonged periods of contact and two brief or distant ones.
The effect this has in practice depends on the nature of the job and the employer. Riddell, the railway conductor and trade union official, says that the proportion of train passengers wearing face masks varies from line to line, but the stretch from Sittingbourne to Sheerness on the west side of Sheppey is particularly risky for rail staff because ‘between 50 and 60 per cent of people, mostly the young ones, don’t wear masks.’ As a conductor, he is allowed stay in the front cabin with the driver and doesn’t have to check passengers’ tickets. But Sue Saunders, who works as a cleaner on the trains, has to walk through the carriages spraying sanitiser and cleaning surfaces. ‘We have visors, masks and gloves,’ she says, ‘but we fear for our safety and several of my friends have caught Covid.’ The cleaners are often the only official-looking people on a train and, according to Saunders, are frequently stopped by passengers who want information. She says that sanitising could be done when the trains are standing empty between journeys, but the train companies want passengers to see that the cleaners are at work.
Compliance with restrictions on social interaction largely lapsed over the summer. Sharon Goodyer, who runs the Margate Food Club, says that her volunteers sometimes couldn’t safely distribute food in poor areas because they had to push past people sitting in doorways and mixing in the street. ‘I have a feeling,’ she says, ‘that if this new variant started in Margate, then we earned it.’ But she points out that even poor people need to get outdoors: ‘You can’t be too judgmental if you’re living in a nice house and don’t have mice dying under your chair.’ Barry Lewis mentions one street in Margate with two hundred overcrowded houses where residents rent tiny rooms at high prices. ‘It’s almost a prison, so to get out to the front of the house is your normal way of life and to be stuck in one overcrowded room is not possible.’
The arrival of the variant changed attitudes. Vanessa Crick, a mother of three in Herne Bay, a rundown town on the coast between Swale and Thanet, has two jobs, in the local library and in a supermarket. ‘Since last November,’ she says, ‘more people have started wearing masks because they are frightened for their granddad or their nan.’ Charlotte Cornell, who runs a charity distributing laptops for homeschooling to children in deprived areas, says that none of the families she deals with is cavalier about the virus: ‘They are all terrified of it.’
When public health experts were sent to Kent at the end of last year to investigate the reasons for the local epidemic, they suspected that the spread would be attributable to human actions at home or in the workplace. Everything they knew about the lives of people in Thanet and Swale would favour accelerated transmission of the virus. The physical environment was a factor too: decayed seaside resorts have many former hotels with sea views whose faded grandeur make them ideal for conversion into care homes. Last May, seventeen residents died from Covid-19 in one such care home in Margate, but mass deaths in care homes were a scandal all over Britain and hardly peculiar to Thanet.
A more likely reason for the rapid spread is that many people had good reasons for not getting Covid tests. People who test positive but need to go out to work and won’t get sick pay can’t afford to quarantine. ‘Young males in economically deprived areas do not want to get tested,’ Jackie Cassell says of Swale. She points to a study in Liverpool where only 4 per cent of people in one of the city’s poorest neighbourhoods volunteered for a test. Since the pandemic began, the government has been voluble about the restrictions it has imposed but evasive about how far people comply with them. A study by King’s College London showed that, while 70 per cent of people said they would self-isolate if necessary, only 18 per cent did so.
People not getting tested because they can’t afford to quarantine will keep a low profile. But other groups aren’t keen to catch the attention of anyone in authority. Graham Tegg, the director of the Kent Law Clinic, which provides free legal assistance, says there is ‘an underground system’ of migrant workers, many of whom have lived in Britain for a long time, who want to keep their distance from state institutions. Many of his clients are Czechs, Poles and Roma. Some pick fruit and vegetables or work in packing factories; collected by minivans in the morning, they work for ten hours and come back in the evening in the same van. ‘Three or four of them may be living in the same small room,’ Tegg says, providing perfect conditions for the virus to spread.
But most people in Thanet and Swale are ‘disconnected from authority’, according to Barry Lewis: the only time they see authority in action is when the police stop them doing something they want to do. Some of them are third-generation unemployed whose only prospect for making money is in the black market or the drugs trade – described by one resident as the only growth industry in Thanet. ‘What we have here is a whole community who have no investment in society at all,’ Sharon Goodyer says. ‘What do they owe anybody? They don’t. They don’t have a decent education, a decent home, a decent job. Why should they behave responsibly?’
Send Letters To:
The Editor
London Review of Books,
28 Little Russell Street
London, WC1A 2HN
letters@lrb.co.uk
Please include name, address, and a telephone number.